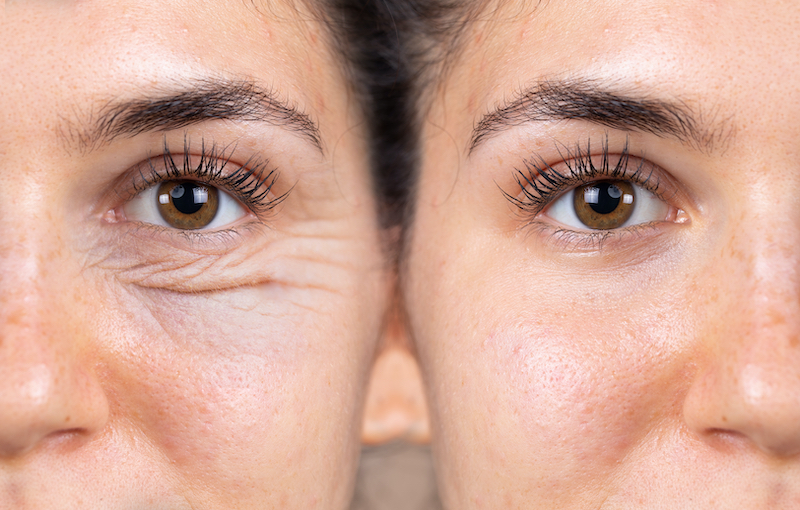
Introduction
Laser skin rejuvenation remains a cornerstone technology in cosmetic dermatology and plastic surgery, providing precise solutions for photoaging, pigmentation disorders, and uneven skin texture. This article synthesizes current comparative evidence on fractional lasers and picosecond lasers, examines the regulatory environment in the United States, explores emerging AI-guided and hybrid technologies, and identifies priority research gaps—particularly inclusivity for different skin tones and the need for long-term research.
1. Evidence Review: Comparison of the Efficacy of Fractional Lasers and Picosecond Lasers in Photoaging and Pigmentation Disorders
Definition and Clinical Scope
Fractional lasers (including ablative and non-ablative types) stimulate collagen remodeling by creating tiny treatment areas. Picosecond lasers, on the other hand, emit ultrashort pulses that primarily break down pigment and tattoo ink through photomechanical effects, with limited thermal damage to surrounding tissue. Both types of lasers are important tools for treating photoaging, acne scars, solar lentigines, melasma, and other pigmentation disorders.
Comparison of Fractional Laser Efficacy in Photoaging and Pigmentation Disorders
Fractal CO2 and fractional erbium lasers demonstrate sustained effects in reducing wrinkles and firming skin by inducing controlled dermal damage and subsequently promoting new collagen production. Meta-analyses of ablative fractional devices show that, using effective scales, objective wrinkle improvement rates typically range from 20% to 50%. Deeper dermal remodeling is associated with higher efficacy but also longer recovery periods and a higher incidence of adverse reactions. Non-ablative fractional lasers (e.g., fractional 1550 nm lasers) offer more favorable recovery curves with moderate clinical improvement and are often chosen by patients seeking shorter downtime and with skin phototypes I–III.
Performance of Picosecond Lasers in Specific Pigmentation Problems
Picosecond devices excel in breaking down pigment particles and tattoo ink through photomechanical effects, achieving faster clearance rates and less associated thermal damage compared to traditional nanosecond Q-switched lasers. Clinical studies and controlled trials report that picosecond lasers can achieve faster pigment removal and reduce post-treatment inflammatory hyperpigmentation in the treatment of pigmented lesions such as nevus of Ota, café-au-lait spots, and refractory actinic lentigines. However, the evidence for the treatment of melasma remains inconsistent—picosecond lasers can reduce epidermal pigmentation, but without strict adjuvant therapy and sun protection measures, the recurrence rate remains high.
Patient Selection Criteria and Evidence-Based Treatment Protocols
The optimal protocol requires comprehensive consideration of the patient's skin phototype, anatomical location, baseline photodamage level, and tolerance to the recovery period. Guidelines supported by clinical studies recommend that for patients with higher skin phototypes (types IV–VI), conservative energy densities and spot testing should be used to minimize the risk of post-inflammatory hyperpigmentation. Typical treatment cycles are: non-ablative fractional lasers typically require 1–3 treatments (4–6 weeks apart), while deeper ablative fractional CO2 lasers require 1–2 treatments (3–6 months apart). For pigmentation removal, picosecond lasers typically require 3–6 treatments, spaced 4–8 weeks apart, depending on the depth of pigmentation. Combination therapy strategies—using fractional lasers to improve skin texture while simultaneously treating pigmentation with picosecond lasers—have shown synergistic effects in specific patient populations, but randomized, head-to-head comparative trials are currently lacking.
2. Regulation, Safety, and Adverse Reactions
In the United States, laser devices are regulated by the Food and Drug Administration (FDA) based on device classification and intended use. While many devices are approved, regulation focuses primarily on the safety and effectiveness of the device, rather than its actual performance in the hands of all populations and operators. This leads to a critical cognitive gap: true clinical outcomes depend heavily on the operator's skill and experience.
Common adverse reactions include transient erythema, edema, and crusting. More serious risks, such as scarring, infection, and, most concerningly, post-inflammatory hyperpigmentation, occur significantly more frequently in patients with darker skin tones (phototype IV–VI). Existing literature often falls short in reporting the racial and ethnic composition of study participants, limiting our ability to generalize these findings and understand true risks. 3. Emerging Technologies and Future Directions
This field is rapidly evolving, with new technologies aiming to improve efficacy, reduce side effects, and enable more personalized treatment.
Artificial intelligence-guided treatments are emerging. By analyzing skin images, AI algorithms have the potential to assist doctors in precise energy delivery, real-time monitoring of the treatment process, and more accurately predicting the effectiveness for individual patients. This could reduce operator variability and improve the consistency of treatment outcomes.
Hybrid technology platforms are emerging, combining different laser wavelengths or energy sources (such as radiofrequency) in the same device. This strategy aims to address multiple skin problems in a single treatment—for example, combining fractional radiofrequency skin tightening and picosecond laser pigmentation removal—providing more comprehensive skin rejuvenation effects and potentially optimizing the patient's treatment process.
4. Research Gaps and Future Directions
Despite significant progress in laser skin rejuvenation technology, several key research areas urgently need to be explored to ensure its safe and effective accessibility for all populations.
The most pressing need is to conduct long-term safety studies on diverse skin types and ethnicities. The current evidence base is severely underrepresented in patients with skin phototypes IV–VI and individuals from diverse ethnic backgrounds. This results in a lack of reliable data for practitioners when treating large populations regarding optimal parameter settings and the risk of long-term complications (such as delayed post-inflammatory hyperpigmentation).
Secondly, more rigorously designed head-to-head clinical trials are needed to directly compare the efficacy, safety, and cost-effectiveness of different laser platforms (especially novel picosecond and fractional lasers) and combination treatment regimens for specific indications (such as different types of melasma).
Furthermore, with the integration of artificial intelligence technologies, it is necessary to study the effectiveness and reliability of these tools in real-world clinical settings and their impact on the shared decision-making process between doctors and patients.
Conclusion
Laser skin rejuvenation provides a powerful tool for addressing photoaging and pigmentation disorders. Fractional lasers have strong evidence for improving skin texture and firming, while picosecond lasers demonstrate unique advantages in pigment removal. However, we should not overlook its "other side": treatment outcomes are highly dependent on the operator, patient selection is crucial (especially in preventing complications in patients with darker skin tones), and there is a significant gap in the diversity of existing research. Future development should focus on improving efficacy and safety through technological innovation, while also conducting more inclusive research to ensure that people of all skin colors and backgrounds can safely and equitably benefit from this technology. In the pursuit of beauty, informed consent, prudence, and inclusion are crucial.